
Isolated infusions
Isolated infusions are another treatment group that is of increasing importance in interventional oncology. In isolated infusions, both the artery and the vein of a particular area or organ in the body are isolated from the systemic circulation. Then, a very high dose of chemotherapy is given via the feeding artery, while the same amount of blood is taken out of the veins. This blood is passed through special filters and the chemotherapy drug is removed, and then the remaining blood is reintroduced into the systemic circulation. In this way, a very high dose chemotherapy (several times higher than intraarterial chemotherapy) is given to the desired region or organ and a high antitumoral effect is achieved, whereas the sistemic side effects are avoided as very little amount of drug is passed into the circulation.
Isolated infusions were first performed surgically, but today, they can be performed in a minimally invasive way by using special catheters, balloons and tourniquets. The most important isolated infusions in interventional oncology are chemosaturation (in the liver) and extremity-pelvis infusions.
Isolated liver infusion (chemosaturation):
Chemosaturation is the most commonly performed isolated infusion therapy. In this procedure, the artery and veins of the liver are separated from the systemic circulation by angiographic methods using special catheters and balloons. Via the artery of the liver, a chemotherapy drug called Melfalan is given to the liver at a very high dose. The same amount of blood from the isolated vein of the liver is taken out of the body. This blood is passed through special filters and more than 99% of Melfalan is filtered out. The filtered blood which is free of Melphalan is then injected back into the circulation via the neck vein. This event is repeated for about 1 hour and all the liver tissue is exposed to very high doses of Melphalan. During the procedure, less than 1% of Melphalan passes into the systemic circulation, which reduces systemic side effects. In chemosaturation, it is necessary to prevent the risk of clotting in vessels as foreign bodies such as multiple catheters and balloons remain in the vessel for more than one hour and some vessels are temporarily blocked. Therefore, during all of the procedure, a very high dose of blood thinner (heparin) must be infused.
Chemosaturation is most commonly performed in liver metastases of the malignant melanoma tumor of the eye (uveal malignant melanoma). In this patient group, in a phase 3 study conducted in 2010, the survival after chemosaturation was approximately 5-times longer than expected. Other local treatments such as chemoembolization and radioembolization in the liver were not as effective as chemosaturation in uveal malignant melanoma metastases.
Chemosaturation has also been tested in other types of liver cancer like cholangiocarcinoma and sarcoma metastases and some success has been obtained. However, there is currently insufficient scientific evidence supporting the use of chemosaturation in such tumors instead of standard treatment methods such as chemoembolization and radioembolization. Therefore, chemosaturation currently should be considered only in those in whom such standard treatment methods cannot be applied or failed.
Isolated leg infusion:
This method is a successful isolated infusion therapy in the skin metastases of malignant melanoma, a common skin cancer, as an alternative to amputation. For the procedure, first the leg of the patient is placed in a special heater bag and the temperature is maintained at about 40 degrees. The goal is to increase the amount of blood coming to the skin by increasing the temperature. Then, a catheter is inserted into the artery and vein of the leg, and a tight tourniquet is applied to the groin to ensure that the leg is completely isolated from the systemic circulation.
After this stage, the blood taken from the leg vein is heated to 40-42 degrees with an external heater and high-dose melphalan is added. If desired, other drugs which are effective in malignant melanoma such as Actinomycin can be added to Melfalan. Then, the warm venous blood containing drugs is injected into the leg artery, thus allowing the leg to be exposed to a very high dose of chemotherapy. During this process, which lasts about 20-30 minutes, both the blood and the leg are heated up to 40-42 degrees, and the skin vessels are expanded and the drug is brought to the skin more and the effectiveness of the drug on the tumors is increased.
Isolated leg infusion is a well-known classic treatment in some major centers in the world. Apart from malignant melanoma metastases, sarcoma tumors were also successfully treated.
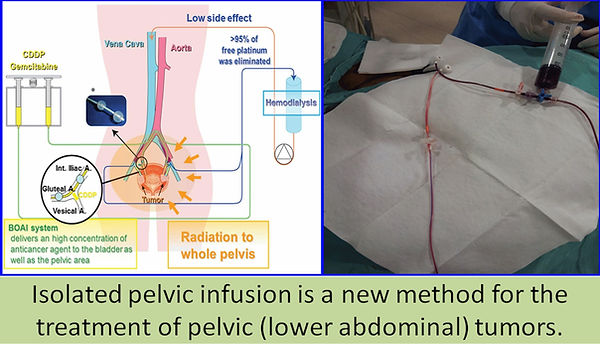
Isolated pelvic infusion:
This is a new isolated infusion therapy that has been introduced in some centers in Japan in recent years. In this treatment, a catheter is inserted via each groin into the inner iliac arteries which feed the organs such as the bladder, rectum or uterus in the pelvis. The veins are also temporarily blocked by inflating a balloon so that the pelvic region is isolated from the systemic circulation. Subsequently, platinum group chemotherapy drugs, such as cisplatin, oxaliplatin, are administered at very high doses into arteries, while venous blood is taken out of the balloon-blocked veins. This venous blood is delivered to the hemodialysis device and the drug (platinum) in it is filtered. The remaining clean blood is given back to the body through the neck vein and the circulation is continued in the normal way. In this way, a very high dose of the chemotherapy drug is given to the tumor in the pelvis, which increases the effect on the tumor and reduces the systemic side effects by preventing the drug from entering the bloodstream.
Isolated pelvic infusion has been used successfully in cervical cancers and bladder cancers. However, the technique has not yet become widespread and its long-term results are not clear. Therefore, its use at this stage is considered experimental.



Interventional oncology in cancer management
Prof Saim Yilmaz, MD


